Tinea capitis in infants in their first 2 years of life: A 12-year study and a review of the literature
Published Web Location
https://doi.org/10.5070/D30519t0b9Main Content
Letter: Tinea capitis in infants in their first 2 years of life: A 12-year study and a review of the literature
Inès Zaraa MD, Abdelmohti Hawilo MD, Sondes Trojjet MD, Dalenda El Euch MD, Mourad Mokni MD, Amel Ben Osman MD
Dermatology Online Journal 18 (7): 16
Dermatology Department, La Rabta Hospital Tunis, TunisiaAbstract
BACKGROUND: Tinea capitis (TC) is a dermatophyte infection that occurs mainly in childhood; but it is uncommon in infants. The aim of this study was to review the clinical and mycological profile of TC in infants. PATIENTS AND METHODS: We present a retrospective study; we enrolled all the cases of infant TC over a period of 12 years (1999-2010). RESULTS: Thirty-five infants (21 boys, 14 girls) with a mean age of 20.16 months were diagnosed with TC among a total number of 881 cases of TC (3.9%). Scalp scaling and alopecia were the most frequent clinical features. Microsporic tinea (21 cases) was the most frequent followed by Trichophytic tinea (9 cases) and inflammatory tinea (5 cases). Direct microscopy of hair was positive in 33 cases (94.2%). Culture positivity was found in 82.8 percent of infants (29 cases). Four species of dermatophytes were isolated; Microsporum canis in 18 cases (62%) followed by Trichophyton violaceum, Trichophyton mentagrophytes, and Trichophyton verrucosum. Twenty-nine infants were treated successfully with griseofulvin. DISCUSSION: TC is rare in infants. The diagnosis of TC should be considered if scaling and/or alopecia are present and should be confirmed by mycology testing prior to initiation of treatment.
Introduction
Tinea capitis (TC) or scalp ringworm is a common dermatophyte infection of the scalp in children [1, 2, 3]. Its occurrence is rare in infants in their first years of life, with only a few reports being available in the literature [4, 5]. Our objective was to review the epidemio-clinical and mycological profile of infant TC diagnosed in our area and compare our results to other series in the literature.
Patients and methods
This retrospective study was performed in the Department of Dermatology of La Rabta Hospital of Tunis, North Tunisia. We reviewed all cases of infants less than 2 years of age with an established diagnosis of TC, who were seen between January 1999 and December 2010 (12 years). The diagnosis of TC was suspected clinically and confirmed by mycological examination (direct examination and/or culture positive). Mycologic investigation, including a direct microscopic mount and fungal culture, was performed for every infant. Clinical material (scales, hair) was used for direct examination with the use of a 30 percent KOH solution. The specimens were also inoculated on Sabouraud 2 percent glucose chloramphenicol agar and Sabouraud 2 percent glucose cycloheximide-chloramphenicol agar.
Results
Epidemiological, clinical features
During the analyzed period of 12 years, a total of 35 cases (2.9 cases/year) were diagnosed with TC among a total number of 881 cases of TC (3.97%). Our patients come from Tunis City in 17 cases (48.6%), a rural region in 11 cases (31.4%), and an urban area surronding Tunis city in 7 cases (20%). A majority of TC were in male infants (57.1%) with a sex ratio (M/F) of 1.33. Patients were between 3 months and 2 years old with a mean age of 20.16 ± 5.64 months (median = 24 months). The mean duration of the disease prior to diagnosis was about 31.7 days ± 27.15 (range 2 days to 3 months; median = 30 days). Other family members presented with TC in 2 cases. Contact with animals was reported in 10 cases (6 cat, 2 dog, 1 rabbit).
 |  |
| Figure 1 | Figure 2 |
|---|---|
| Figure 1. Alopecic patches of the hair Figure 2. Diffuse scaling of the hair | |
 |
| Figure 3 |
|---|
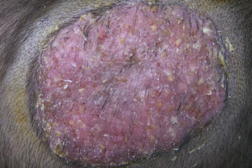
| Figure 3. Follicular pustular elements on squamous erythematous alopecic patches, suggesting a kerion |
“Alopecic patch” was the most common clinical type (17 cases: 48.57%) (Figure 1), followed by diffuse scaling of the hair at follicle level (13 cases: 37.14%) (Figure 2). Five infants had follicular pustular elements on squamous erythematous alopecic patches, suggesting a kerion (Figure 3). No case of favus was seen. Physical examination showed tinea corporis in 2 cases (face: 1 case, trunk: 1 case). The characteristics of our study are represented in Table 1.
Mycological features
Direct examination was positive in 33 cases (94.28%); it showed ectothrix invasion in 27 cases (81.8%) and endothrix in 6 (18.2%) samples. The distribution of the different species according to sex is presented in Table 2. Positive cultures of dermatophytes were obtained in 29 infants (82.8%): Microsporum canis (18 cases; 62%) was predominant. The relationship between direct examination and culture is represented in Table 3.
Treatment and follow-up
Treatment regimen consisted of griseofulvin at the dose of 15 mg/kg/d for 6-12 weeks, associated with antifungal topicals for all infants except five (less than 6 months of age), which were treated just by antifungal topicals. The tolerance of treatment was excellent and no side effects or abnormal results in blood chemistry tests were observed. A systemic antibiotic and prednisone (0.5 mg/kg/daily) were given to the 2 patients with kerion. A limited shaving of the plaques was made in all our infants. The follow-up in 30 infants showed complete hair regrowth in 28 cases; 2 cases of kerion showed persistent alopecia.
Discussion
TC is a dermatophytosis of the scalp and hair that appears most often in children between 3 and 7 years of age and is rare in the first years of age. Only a few articles in the literature discuss this population and most of them are case reports [6-12]. Romano et al. published the most exhaustive study of dermatophytosis in infants, including 15 cases diagnosed in Italy [4]. In our study, 35 cases (3.9%) of TC were reviewed among a total 881 TC collected through 12 years.
Some authors suggest that TC in infants occurs more in boys than in girls. This seems to be related to the etiological agent because M. canis are more prevalent in boys, whereas there is no predominant gender for TC caused by T. violaceum [4, 5]. In our study, we found a predominance of cases in boys for TC produced by both M. canis (11/18 cases) and by T. violaceum (7/9 cases).
The most reported factors predisposing infants to TC are humid environment, broad-spectrum antibiotic use, epidermal immaturity and impairment of health (anemia, immunodepression) [13]. It has also been proposed that asymptomatic carriers (mothers), without clinical signs or symptoms of TC but with positive scalp cultures, could be an important source of disease transmission or a reservoir of dermatophytes [4]. Clinically, infant TC is extremely variable, presenting problems for diagnosis [14, 15]. Diagnosis is easy in the case of typical Microsporum or Trichophyton TC; it is more difficult in cases with clinical manifestations resembling pseudotinea amiantacea, seborrheic dermatitis, bacterial folliculitis, or pustular psoriasis, which are often treated incorrectly [16, 17, 18]. The most frequent clinical features in our study were “alopecic patches,” present in 17 cases (48.57%). Scaling was the sign most frequently reported in the literature [5].
TC is a classic example of the changing geographic patterns of dermatophytosis, which explains the polymorphisms of clinical and mycological profil of TC [19, 20]. In our study, the predominant agents were zoophilic dermatophytes, especially M. canis, which is consistent with most reports in the literature. This significant increase, also reported in North Africa and in many Mediterranean countries, could be explained by the high frequency of domestic animals (especially cats and dogs) in large cities. [21, 22]. T. violaceum seemed to be found more rarely. Our data showed 9 cases of T. violaceum [23, 24]. Although, in most patients with an anthropophilic dermatophyte, a family member was the source of infection. T. mentagraphytes and T. verrucosum (1 case each) were occasionally isolated in the literature.
Since the 1950s, griseofulvin has been the drug of choice for the treatment of TC in infants because of its efficacy, low cost, and excellent safety profile [25]. It has been used previously in newborns and tolerated well. Our infants were treated by griseofulvin (15 mg/kg/d for 6-12 weeks) associated with antifungal topicals for all infants except five (less than 6 months of age), which were treated just by antifungal topicals with good results. A favorable response to topical antifungals has already been reported in TC in infants under 3 months. However, more studies are needed before accepting topical antifungal alone as a proper treatment for TC in infants.
The newer antimycotic drugs (fluconazole, terbinafine, itraconazole) are well documented in treating TC especially in children older than 1 year of age but has not obtained approvaql for TC in Tunisia [26-31].
Conclusion
TC is rare in early infancy. The microsporic and trichophytic are the most frequent forms. Although it occurs infrequently, the diagnosis of TC should be considered when an infant presents with scaling or alopecic patches on the scalp and should be confirmed by mycology prior to initiation of treatment.
References
1. Makni F, Néji S, Sellami A, Cheikhrouhou F, Sellami H, Marrakchi S, et al. Les teignes du cuir chevelu dans la région de Sfax (Tunisie). J Mycol Med 2008; 18: 162-5.2. Rebollo N, López-Barcenas AP, Arenas R. Tinea capitis. Actas Dermosifiliogr 2008; 99: 91-100. [PubMed]
3. Boumhil L, Hjira N, Naoui H, Zerrour A, Bhirich N, Sedrati O, et al. Les teignes du cuir chevelu à l’hôpital militaire d’instruction Mohammed V (Maroc). J Mycol Med 2010; 20: 97-100.
4. Romano C, Gianni C, Papini M. Tinea capitis in infants less than 1 year of age. Pediatr Dermatol 2001; 18: 465-468. [PubMed]
5. Gilaberte Y, Rezusta A, Gil J et al. Tinea capitis in infants in their first year of life. Br J Dermatol 2004; 151: 886-890. [PubMed]
6. Eleuch D, Mokni M, Sellami A, Cherif F, Azaiz MI, Ben Osman Dhahri A. Les teignes du cuir chevelu observées à Tunis de 1985 à 1998 : à propos de 1222 cas. J Mycol Med 2001; 11: 87-91.
7. Monteagudo B, Pereiro M Jr, Pereiro C et al. Tinea capitis en el a´rea sanitaria de Santiago de Compostela. Actas Dermatosifiliogr 2003; 94: 598-602.
8. Gilaberte Y, Rezusta A, Coscojuela C. Tinea capitis in a newborn infected by Microsporum audouinii in Spain. J Eur Acad Dermatol Venereol 2003; 17: 227-249. [PubMed]
9. Hubener LF. Tinea capitis (Microsporum canis) in a thirty-day-old infant. AMA Arch Derm 1957; 76: 242. [PubMed]
10. Zaror L, Moreno MI, Bilbao MT. Tinea caused by Microsporum canis in children under 30 days of age. Sabouraudia 1985; 23: 1-5. [PubMed]
11. Baudraz-Rosselet F, Ruffieux C, Grigoriu D. Microsporum infection in a 3-month-old infant. Ther Umsch 1984; 41: 403-5. [PubMed]
12. Bereston ES, Robinson HM Jr. Tinea capitis and corporis in an infant four weeks old. AMA Arch Derm Syphilol 1953; 68: 582-3. [PubMed]
13. Smolinski K, Shah S, Honig P et al. Neonatal cutaneous fungal infections. Curr Opin Pediatr 2005;17: 486-493. [PubMed]
14. Cabon N, Moulinier C, Taieb A, Maleville J. Microsporum langeronii dermatophytosis in a newborn infant contaminated in France. Ann Dermatol Venereol 1994;121: 247-8. [PubMed]
15. Alteras I, Feuerman EJ, Grunwald M, Shvili D. Tinea capitis due to Microsporum canis in infants. Mycopathologia 1984 30; 86: 89-91. [PubMed]
16. Weston WL, Morelli JG. Neonatal tinea capitis. Pediatr Infect Dis J 1998;17: 257-8. [PubMed]
17. Koussidou-Eremondi T, Devliotou-Panagiotidou D, Mourellou-Tsatsou O, Fotidou D, Minas A. Tinea capitis in children in northern Greece during the period 1981-1995. Mycoses 1999;42: 319-22. [PubMed]
18. Bigel ML, de France-Pinchon C, Richardin F, Furioli J, Bourgeois-Droin C. Tinea capitis presenting as staphylococcal pyodermatitis of the scalp. Arch Fr Pediatr 1989 ;46: 363-5. [PubMed]
19. Aly R, Hay RJ, Del Palacio A, Galimberti R. Epidemiology of tinea capitis. Med Mycol 2000; 38: 183-188.
20. Fuller LC. Changing face of tinea capitis in Europe. Curr Opin Infect Dis 2009 ;22: 115-8. [PubMed]
21. Mebazaa A, Oumari KE, Ghariani N, Mili AF, Belajouza C, Nouira R, Denguezli M, Ben Said M. Tinea capitis in adults in Tunisia. Int J Dermatol 2010; 49: 513-6. [PubMed]
22. Razzaq Adel AA, Sultan AO, Basmiah AM, et al. Prevalence of tinea capitis in southern Kuwait. Mycoses 2007; 50: 317-320. [PubMed]
23. Surpam RB, Deshpande SD, Saraswathi K, Amladi S, Savant S. Trichophyton violaceum : A rare isolate in 18-day-old neonate. Indian J Med Microbiol 2006; 24: 292-3. [PubMed]
24. Ghorpade A, Ramanan C. Tinea capitis and corporis due to Trichophyton violaceum in a six-day-old infant. Int J Dermatol 1994; 33: 219-20. [PubMed]
25. Kakourou T, Uksal U; European Society for Pediatric Dermatology. Guidelines for the management of tinea capitis in children. Pediatr Dermatol 2010; 27: 226-8. [PubMed]
26. Valari M, Iordanidou A, Raftopoulou A, Pangalis A. Fluconazole in the treatment of pediatric tinea capitis caused by Microsporum canis. Drugs Exp Clin Res 2002; 28: 161-4. [PubMed]
27. Baudrez-Rosselet F, Monod M, Jaccoud S, Frenk E. Efficacy of terbinafine treatment of tinea capitis in children varies according to the dermatophyte species. Br J Dermatol 1996;135: 1011-2. [PubMed]
28. Binder B, Richtig E, Weger W, Ginter-Hanselmayer G. Tinea capitis in early infancy treated with itraconazole: a pilot study. J Eur Acad Dermatol Venereol 2009; 23:1161-3. [PubMed]
29. Ginter-Hanselmayer G, Smolle J, Gupta A. Itraconazole in the treatment of tinea capitis caused by Microsporum canis: experience in a large cohort. Pediatr Dermatol 2004; 21: 499-502. [PubMed]
30. Gupta AK, Cooper EA, Ginter G. Efficacy and safety of itraconazole use in children. Dermatol Clin 2003; 21: 521-35. [PubMed]
31. Koumantaki E, Georgala S, Rallis E, Papadavid E. Microsporum canis tinea capitis in an 8-month-old infant successfully treated with 2 weekly pulses of oral itraconazole. Pediatr Dermatol 2001; 18: 60-62. [PubMed]
© 2012 Dermatology Online Journal

